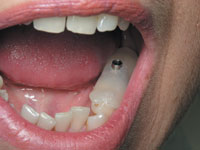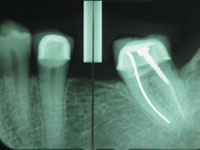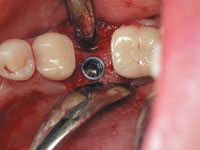
Dental Implant stent
 Restorative dentists have an essential role in the diagnosis of the restorative needs of patients treated with dental implants.1 An implant template is the means of communication used to transfer positioning requirements to the surgeon, who can then place the implants in positions that allow for ideal restoration of the occlusion.2 Templates are necessary even for single implants.3
Restorative dentists have an essential role in the diagnosis of the restorative needs of patients treated with dental implants.1 An implant template is the means of communication used to transfer positioning requirements to the surgeon, who can then place the implants in positions that allow for ideal restoration of the occlusion.2 Templates are necessary even for single implants.3
According to Misch, the surgical template dictates to the surgeon the implant placement that offers the best combination of (1) support for the repetitive forces of occlusion, (2) aesthetics, and (3) hygienic requirements.4 A well-designed template can reduce surgical time, improve the accuracy of implant placement, reduce the need for expensive, vector-changing abutments, and improve the aesthetic emergence profile of the restoration.
There are a variety of template types, ranging in sophistication and cost from inexpensive vacuum-form shells to computerized tomography (CT)/computer-derived templates. The following types of implant templates have been used:
Restorative implant templates indicate the shape and position of the proposed restoration(s) but do not dictate the osteotomy path for the surgeon. These are generated from diagnostic models and generally include (1) vacuum-form duplicates of diagnostic models, (2) acrylic resin material based on a diagnostic wax-up, or (3) direct resin adaptation to the diagnostic model. Each of these templates cover the occlusal tables of adjacent teeth for support. The proposed implant site is often represented in acrylic on the restorative template by the facial surface of the desired restoration or by the intact acrylic representation of the entire proposed restoration for the surgeon to manipulate as is appropriate.
The advantages of restorative templates are their ease of fabrication, commonly available materials and techniques, and low cost. The disadvantage of the restorative template is that it does not dictate the position of the osteotomy.
 Surgical implant templates may also indicate the shape of the proposed final restoration but dictate the osteotomy as well. They are generally based on CT scan data and computer-driven design and fabrication. In this category, a CT scan is taken of the patient's jaw. The implant surgery is planned using CT scan, and a computer-assisted process relates the proposed axial and depth alignment. Surgical CT-based templates are generally fabricated by 1 of 2 processes: (1) CAD/CAM (Computer-Assisted-Design-Computer-Assisted Manufacture) milling, and (2) stereo-lithography.
Surgical implant templates may also indicate the shape of the proposed final restoration but dictate the osteotomy as well. They are generally based on CT scan data and computer-driven design and fabrication. In this category, a CT scan is taken of the patient's jaw. The implant surgery is planned using CT scan, and a computer-assisted process relates the proposed axial and depth alignment. Surgical CT-based templates are generally fabricated by 1 of 2 processes: (1) CAD/CAM (Computer-Assisted-Design-Computer-Assisted Manufacture) milling, and (2) stereo-lithography.
The advantages of using surgical templates include predictability of placing implants in proper alignment, avoiding injury of adjacent structures (teeth, sinuses, or cortical plates), and reduced surgical time, 5 with corresponding improvement in postoperative healing. The disadvantages of using surgical templates are the higher start-up costs of computer software and the learning curve associated with reading CT scans and creating the correct treatment plan. Furthermore, dentists might hesitate to utilize surgical templates because of the added expense and inconvenience to the patient, especially for less involved cases.
 Therefore, restorative templates are quite simple, while surgical templates are more complex. The effort the restorative dentist invests in designing and fabricating an implant template, and the type of template selected, should reflect information that should be transferred to the implant surgeon to assure a successful prosthetic outcome.
Therefore, restorative templates are quite simple, while surgical templates are more complex. The effort the restorative dentist invests in designing and fabricating an implant template, and the type of template selected, should reflect information that should be transferred to the implant surgeon to assure a successful prosthetic outcome.
For implant treatment consisting of one to a few implants, dentists may be able to communicate the necessary information adequately with the simpler restorative template. Nevertheless, relatively simple cases can have only a small margin of error. Each implant and restoration has a set of challenges determined by location, hard- and soft-tissue anatomy, spacing between adjacent teeth, and other aspects of local anatomy involving location of neurovascular bundles, sinuses, and cortical plates of bone. Predetermining the appropriate osteotomy path for the surgeon could greatly assist the surgical procedure.
A type of template that is seldom used but has advantages of both the restorative and surgical templates is the surgical guide-tube template. It is fabricated as a restorative template with a hard resin material that rests on the occlusal table of adjacent teeth. As opposed to relying on a CT scan, the restorative and surgical considerations are related by bone mapping and radiographic verification.
This article will present a technique for fabricating guide-tube templates, including verification of accuracy and guidelines for use during implant surgery.
MATERIALS AND METHODS
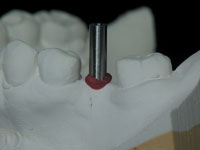
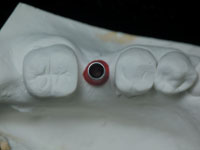
| Figure 1. Surgical guide-tubes (Stent Guide Tubes, 3i Implant Innovations Corp). |
Guide-tubes are prefabricated, stainless steel, radiopaque tubes that can be obtained from implant manufacturers (eg, Stent Guide Tubes, 3i Implant Innovations, Figure 1). They are manufactured with only a single internal diameter of approximately 2.3 mm, which accommodates only the initial size osteotomy burs, and a length of 10 mm that can be trimmed to fit the thickness of the template or to accommodate the vertical space necessary for the surgical handpiece. The guide-tubes are embedded into acrylic models via laboratory acrylic processing or by a direct acrylic process on models.
Implant surgery begins with the creation of a small diameter osteotomy. Guide-tubes will dictate the path of these initial burs. After the initial osteotomy is prepared, the template is removed from the mouth and subsequent larger diameter burs tend to follow the path initially created. To relate the access tube properly in the buccal-palatal/lingual dimension of bone, one additional diagnostic step (bone mapping) is necessary to predetermine the outer dimensions of the cortical plates of the implant site.