Risks of Dental Implants
 Ok let’s face it, any surgical operation has its inherent risks and problems. And the same can be said about dental implant operation.
Ok let’s face it, any surgical operation has its inherent risks and problems. And the same can be said about dental implant operation.
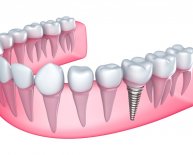
For most cases, dental implants are a no-brainer choice when it comes to replacing a missing tooth or teeth, by using implants as roots to anchor teeth into the jawbone.
The average sucess rate is pretty impressive, which is about 95%. It can even go as high as 98% with some very experienced and skilled dentists.
By the way, if your dentist assures you implants are 100% successful, then alarm bells should start to ring, and you should probably seek another dentist.
In fact, there is 5 or 2% failure that you must be aware of.
Most of those failures are caused by bad planning or uncomplete assessment of the patient’s bone conditions, which is often associated with a lack of skills or inexperienced dentists. But fortunately, most issues can be easily solved if corrrective actions are taken quickly.
I know that no one wants to know or hear about those complications but when taking a decision, you need to see the whole picture with the pros and the cons. That is the wisest way to to go.
Besides, the more you know about possible complications, the more you can help monitor the evolution of your implants and alert your dentist if you notice something wrong. That is the best way to avoid further complications.
Implant is loose or is falling out
This is probably the main dental implant problems. This happens when the bone does not grow and fuse with the implant (between the threads of the implant).
This is what we call the osseointegration failure. You know by now, osseointegration is the process by which the dental implant material fuses with the bone. This process is usually completed within a few months, resulting in a strong and tight connection between the implant and the jawbone. So, the implant is tightly fixed to the jawbone and won’t move when chewing.
If this process does not occur correctly, your dental implant will not function properly. It will become uncomfortable, become loose, or fall out completely.
Bone loss after the implant is placed, is also another indicator. Bone loss of less than 0, 2 millimeter a year after the operation is tolerable; more than that, it would be considered a failure.
Keep in mind some slight bone loss over many years is normal, which can be considered normal age-related bone loss, but it shouldn’t affect your implants directly.
What are the main reasons of failed ossointegration?
- Inaccurate positioning: a faulty alignment of the implant can lead to forces that can prevent the bone to sucessfuly grow around it.
- Excessive loading or overloading: the functional load applied to the implant exceeds the capacity of the bone to support it and affects the bone growing.
- Volume or density insufficiency of the bone
- Damage to the tissue surrounding the implant
- Oral or intravenous bisphosphonates (fosamax, actonel or boniva) that can affect the ability of the jawbone to heal
- Blunt force trauma that affects the healing and bone integration process
- Formation of a thin fibrous capsule around the implant
- Dental implant Inflammation
- Infection
If osseointegration does not take place, the dental implant can be removed, and surgery can be attempted again once the implant area has fully healed.
This illustrates why the assessment of your jawbone is certainly the most important part of the procedure because if your dentist tries to place implants in a « weak » jawbone, then you can expect a higher rate of failure.
Prior to the operation, the dental specialist must first establish the integrity of your jawbone to support the implant. Measurements of your bone’s height, width, and density are taken to make sure that it can hold the implant in place.
If necessary, procedures like bone grafting or sinus lift (a bone grafting in the sinus area) will be required to ensure that you have a solid bone mass that will support osseointegration.
Overloading : when impatience leads to dental implant problems
Overloading has been listed above as a failed ossointegration cause; I wanted to give you a little more details about this issue.
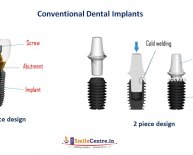
So what is it? Overloading is a result of applying severe pressure on the area of dental implant operation. This is most commonly observed in implants where the implant (the post or the screw part) and the abutment are placed at the same time. (Remember the 3 stages of a dental implant operation?)
On this procedure, the abutment protrudes out of the gum while the implant is still in the process of osseointegration. So it means extra care is needed when you opt for this procedure because any pressure exerted on the abutment during the healing process will cause further injury and may actually prevent full integration of the bone and the implant. That means a bad ossointegration and a loose implant as a result.
If you are sure that you will be able to take good care of your implant, this all-in-one procedure may save you a lot of time because you will have 2 procedures done in one operation.
But if you consider long-term safety and benefits, you’d better be on the safe side by undergoing a 3-stage dental implant procedure where the implant (post or screw part) is placed first. You would wait for 3-4 months for the bone to fuse with the implant, then the dentist would set up the abutment and then the crown. It is a bit longer but it is worth sometimes to wait longer for a more successful implant surgery.
Fosamax, actonel, boniva : possible complications with biphosphonates
You know dental implants need to be fully integrated to the jawbone to be considered a success, so as you can imagine any medication that affects the bone healing process, might be an issue to get these implants perfectly embedded in the bone.
Still not clear?
These drugs actually prevent bone from breaking down so as a net result the bone density or thickness increases.
But then what is the problem? When you have dental implants, the dentist will make holes to insert the implants, so he or she will kind of break your bones. These bones will have to grow into the implant. Yet bone healing is a complex process that involves breaking (or resorbing) and bone forming, it is more of a bone remodeling process. So because biphosphonates inhibit the bone resorbption phase, these medications will prevent the bone to heal normally and lead to what dentists call jaw osteonecrosis.
What is jaw osteonecrosis? This is a destructive process of the jawbone, with the bone being exposed in the mouth and the gum doesn’t heal over it.
So what are your options?
Well there are 2 cases:
- If you take biphosphonates intravenously, then the dental implant procedure is more at risk, so it is in most cases contraindicated
- If you take them orally, then you have more chances to get implants. Yet, the risk of osteonecrosis is less high depending on the treatment duration. The longer the treatment prior to the considered implant operation, the higher the risk. If you have taken oral biphosphantes for less than 3 years, then the risk is lower.
Whatever your personal situation, please keep in mind nothing is all black or white and some dentist have had great results even with patients with biphosphonates treatment. Nothing is set in stone. Let simply your dentist check your risk and give you his or her personal opinion on your rate of success.
This also highlights the importance of giving your complete medical and dental history, so your dentist gets all the elements to better assess your risks.
See also:
- Pelajari lebih lanjut di https://affaires-dz.com/ hari ini juga.